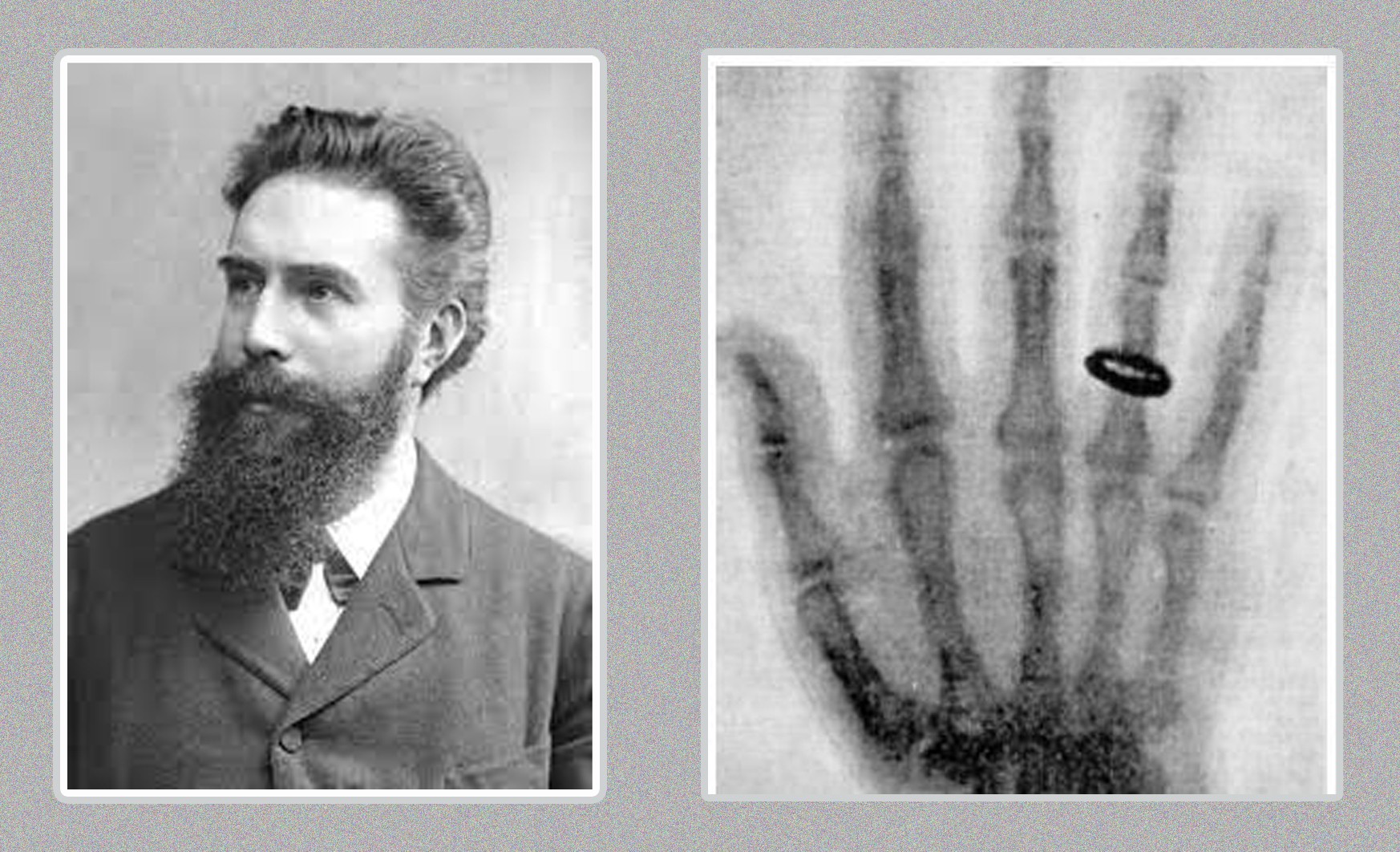
In November 1895, German engineer and physicist Wilhelm Rontgen was experimenting with electrons in his laboratory when he noticed a glowing effect caused by mysterious rays that seemed to pass through solid objects. That timely observation changed medicine forever. Over the next 130 years, radiology evolved from a single discovery into a complex family of medical imaging specialties including X-ray, fluoroscopy, CT, MRI, ultrasound, nuclear medicine, PET, interventional radiology, and now AI-powered diagnostic tools. This blog post walks us through that transformation chronologically, explains how each radiology modality works, highlights major milestones, and outlines current trends and implications for clinicians, patients, and allied health professionals.
Early Discovery and Clinical Adoption, 1895–1920
1895: Wilhelm Rontgen discovered X-rays while experimenting with cathode rays. He observed that these unknown rays produced fluorescent effects on a nearby surface and eventually produced the first radiograph, an image of his wife’s hand wearing a ring. This novel discovery introduced the possibility of seeing inside the living body without cutting it open.
1896–1910: These early years were characterized by rapid clinical adoption. Within months of his discoveries being publicized, physicians worldwide began using X-rays to locate bullets, fractures, and foreign bodies. Early radiography used glass photographic plates or film and required long exposure times.
Early challenges: Included lack of understanding about radiation risks, inconsistent image quality, and primitive diagnostic imaging equipment. Protective measures against radiation exposure were minimal in this period.
Interwar and Early Technology Improvements, 1920s–1940s
New techniques: The eventual introduction and refinement of fluoroscopy provided for real-time imaging of motion and contrast studies. Improvements in X-ray tubes, faster film, and image intensifiers gradually reduced exposure times and improved diagnostic utility.
Contrast agents: Barium sulfate became a standard for gastrointestinal radiography. Iodinated contrast agents for vascular and organ visualization were also developed and refined.
By mid-20th century, radiology had become an established medical specialty with dedicated departments and radiographers.
Midcentury Breakthroughs: Ultrasound and Nuclear Medicine, 1940s–1960s
Sonography: Diagnostic ultrasound evolved from sonar technology and was applied to medicine in the 1940s and 1950s. Early ultrasound found use in obstetrics and abdominal imaging, providing a non-ionizing alternative for many exams.
Nuclear medicine: The development of radioisotopes led to functional imaging of internal organs. Radionuclide techniques allowed assessment of organ function, not just structure. Technetium-99m later became a central tracer due to favorable properties, and nuclear medicine departments grew to provide cardiac, bone, thyroid, and renal scans.
These radiology modalities introduced a new concept: diagnostic imaging to measure physiology and function, not only anatomy.
The CT and MRI Revolutions, 1970s–1990s
CT (computed tomography): In the early 1970s, CT scanners were introduced. CT transformed diagnostic imaging by producing cross-sectional views of the body with superior contrast resolution for soft tissues compared to conventional radiography. CT rapidly became essential in trauma, neurology, oncology, and many other medical fields.
MRI (magnetic resonance imaging): Developed from advances in nuclear magnetic resonance physics, MRI provided detailed soft-tissue contrast without ionizing radiation. Clinical MR scanners entered practice in the 1980s and opened entirely new diagnostic possibilities for brain, spine, musculoskeletal, and pelvic imaging.
These two innovative technologies reshaped diagnostic pathways and contributed to specialization within radiology.
Digital Transformation, PACS, and Teleradiology, 1980s–2000s
Digital radiography and PACS: Traditional film gave way to digital detectors and Picture Archiving and Communication Systems. PACS allowed digital images to be stored, retrieved, and distributed electronically, enabling remote reading and streamlined workflows.
Teleradiology: With digital images, radiologists could read studies remotely, allowing for off-hours coverage, sub-specialist reads, and global reporting services.
These major shifts changed infrastructure requirements, staffing models, and business models for radiology services.
Interventional Radiology and Minimally Invasive Therapies
Therapeutic applications: Interventional radiology emerged as a therapy-focused branch that uses image guidance to perform minimally invasive surgical procedures such as angioplasty, embolization, stent placement, biopsies, and tumor ablation.
Interventional techniques reduced morbidity and hospital stays and expanded the role of radiology from diagnosis to treatment.
PET, Hybrid Imaging, and Molecular Imaging
Positron Emission Tomography (PET): PET allows diagnostic imaging of metabolic and molecular processes. FDG-PET became a cornerstone of oncology imaging.
Hybrid imaging: PET-CT and PET-MRI combine anatomical and functional medical imaging, improving lesion localization and characterization.
Molecular imaging continues to expand with novel tracers for targeted diagnostics and theranostics.
Radiation Safety, Regulation, and Contrast Agent Evolution
Regulation: As imaging modalities spread, awareness of radiation risks increased. Professional organizations and regulatory bodies established guidelines for dose optimization, quality assurance, and safe practice.
ALARA: This principle, which stands for “as low as reasonably achievable,” became central to radiation protection, meaning to minimize exposure to the extent possible.
Agent improvements: Contrast agents evolved from early barium and primitive iodinated agents to safer, higher-quality iodinated agents and gadolinium-based MRI agents, followed by increased scrutiny around gadolinium retention and safety.
Regulatory bodies like the FDA, International Commission on Radiological Protection (ICRP), and national commissions shaped safety, equipment standards, and training.
The 21st Century: AI, Precision Imaging, and Patient-Centered Care
Artificial intelligence: Machine learning and deep learning have been applied to image analysis, triage, quality control, workflow automation, and image reconstruction. AI assists radiologists, helps prioritize urgent studies, and improves detection of subtle findings.
Personalized and precision imaging: Medical imaging increasingly drives targeted therapies, image-guided biopsies, and theranostics that combine diagnosis and therapy.
Patient experience: Faster scanners, noise reduction in MRI, lower doses in CT, and patient-centered scheduling and reporting have improved patient comfort and throughput.
Workforce and training: Subspecialization, remote reading, and multidisciplinary teams are shaping radiology career paths and staffing needs.
Timeline: Key Dates and Milestones in Radiology
- 1895: Wilhelm Rontgen discovers X-rays and produces first radiograph.
- 1896 onward: Rapid adoption for fracture, foreign body, and surgical localization.
- 1920s–1940s: Fluoroscopy advances; contrast studies improve.
- 1940s–1950s: Diagnostic ultrasound begins medical use.
- Mid-20th century: Growth of nuclear medicine with radioisotopes.
- Early 1970s: Clinical CT scanners introduced, enabling cross-sectional imaging.
- 1980s: Clinical MRI enters practice for high-contrast soft tissue imaging.
- 1980s–1990s: PACS and digital radiography replace film in many centers.
- 1990s–2000s: PET-CT and hybrid imaging appear.
- 2000s–present: Interventional radiology expands; AI begins to enter clinical workflows.
Important Radiology Pioneers:
- Wilhelm Rontgen – discovery of X-rays.
- Godfrey Hounsfield and Allan Cormack – early CT pioneers.
- Paul Lauterbur and Peter Mansfield – key figures in MRI development.
- Charles Dotter – pioneer of angioplasty and interventional techniques.
Many clinicians, physicists, technologists, and engineers contributed to the field of radiology through the 20th century to the present.
How Each Major Imaging Modality Works
- X-ray: Ionizing radiation passes through the body and produces a 2D projection; dense structures like bone absorb more X-rays and appear white.
- Fluoroscopy: Real-time X-ray imaging for motion and interventional guidance.
- Computed Tomography (CT): Multiple X-ray projections are obtained and reconstructed to form cross-sectional images. Excellent for trauma and chest/abdominal imaging.
- Magnetic Resonance Imaging (MRI): Uses magnetic fields and radiofrequency pulses to produce high-contrast soft-tissue images without ionizing radiation.
- Ultrasound: High-frequency sound waves create images; safe and real-time, widely used in obstetrics, cardiology, and abdominal imaging.
- Nuclear medicine / PET: Radioactive tracers show physiological processes. PET often uses FDG to show metabolic activity, critical in oncology.
- Interventional Radiology: Uses imaging guidance to perform minimally invasive medical procedures.
Where the Radiology Field Is Headed
- AI integration: From image triage to assisted diagnosis and report automation.
- Faster, lower-dose imaging: Ongoing advances in detector technology and reconstruction algorithms.
- Molecular imaging and theranostics: New tracers and paired therapy strategies.
- Point-of-care ultrasound: Continued growth in bedside imaging by non-radiologist clinicians.
- Remote and distributed care: Greater use of teleradiology for subspecialist reads and 24/7 coverage.
- Workforce evolution: More hybrid roles, cross-training, and demand for technologists with digital and AI-savvy skills.
Are you a medical imaging clinician looking for travel assignments or per diem work? Apply now to speak with a radiology recruiter about current and future openings.